|
Patient engagement is active collaboration between patients and providers. Patients who are engaged in their healthcare tend to have better health outcomes because they trust their providers and the care provided to them. Ultimately, they have greater satisfaction than those who are not engaged in their healthcare decision-making process. Satisfied patients drive reimbursements because they share their experiences with others. Hence, healthcare leaders and the staff must spend effort to increase patient engagement in the following ways:
1. Give patients online access to medical records According to a study conducted by Accenture, 57% of patients say that they can manage their health properly and get more engaged if their medical records are available online. 41% of patients were willing to switch physicians if they can get online access to their medical records. This is one of the top demands of patients nowadays. 2. Use email to communicate Catalyst Healthcare Research found that 93% of the patients would prefer a doctor who offers email communication. Providers can create an email list for sharing updates, marketing their practice, educating and providing health information to patients and much more. They can remind patients about their appointments via e-mail instead of phone calls. 3. Recommend mHealth applications According to a survey conducted by Research Now, 46% of clinicians believe that mHealth apps improve patient engagement and 86% believe that health apps help them increase their knowledge of their patients’ conditions. 96% of patients said they believe mHealth apps would help them improve their care. 9/10 patients said that if their physician prescribed an app, they'd use it. MHealth apps allow patients to monitor their health and report symptoms to their physicians with ease, allowing them to get involved in their care. 4. Offer Virtual Visits According to a survey, 75% of patients who haven't used telemedicine before, said they were interested in trying it as an alternative to an urgent care visit. With majority of the people having a smartphone nowadays, providers can improve their margins, reduce cost, and connect frequently with patients by offering virtual visits. 5. Make your website mobile-friendly Approximately 64% of adult Americans own a smartphone. People use their phones throughout the day. Providers can communicate and engage their patients by making their website mobile-friendly so that they can easily search information. Moreover, providers can develop their own mobile app through which they can send appointment reminders, educate their patients, provide daily medication reminders, etc. 6. Build Online Presence Studies show that 62% of patients see online reviews to find a new doctor. Physicians can build their online presence via blogs, social media websites, etc. which will attract new patients, help the physicians in building a relationship of trust with their existing patients and increase their reputation. 7. Engage senior patients through technology It is a myth that senior patients don’t use technology to manage their health. 84% of baby boomers use internet to search medications and get information about medical conditions. According to a survey, 57% of seniors wanted to interact with their physician and manage their health online. Hence, providers can use technology to engage their senior patients too. 8. Help patients stay in touch Organizations must provide call service and strong internet connection so that patients can communicate with their loved ones through Skype or other applications. This will help in quick recovery of the patients. 9. Organize support groups In-person support groups for the patients and their loved ones or links of online support groups can be provided to the patients so that stay involved in their care. 10. Reward the patients Giving small gifts, discounts, coupons etc. to those patients who achieve certain health outcomes will motivate them to engage and be more serious about their health. Source:
0 Comments
With a shift from fee-for-service to value-based reimbursement, it is imperative for healthcare organizations to improve their revenue cycle performance in order to earn higher margins. Value-based care demands reduction in costs, focus on population health and delivery of high quality health services to all the patients. These goals can have a significant impact on revenue cycle, but healthcare organizations can achieve these goals without a reduction in their margins by:
1. Analyzing appropriate data to track performance: Key performance indicators (KPIs) must align and support every aspect of the revenue cycle. The leaders and the finance people must use advanced data analytics and regularly review the data to know where their revenue cycle is trending and what actions should they take to improve it. The organization can use digital dashboards to show the trend of the KPIs and how they compare with the industry benchmarks. This will help the leaders in identifying the troublesome areas that can have an impact on the organization’s bottom-line. 2. Creating a revenue cycle team of key people: The dashboard showing KPIs can only be useful if key people effectively use it to make decisions for the improvement of the revenue cycle. A committee should be created consisting of the shareholders, executives, clinicians, and financial leaders. The committee members must have access to the digital dashboard so that they are aware of the major issues and can decide how to improve certain things like billing, coding, claim denial, etc. 3. Identifying strengths and weaknesses: It’s not necessary that every organization must have the capability and expertise to resolve various issues regarding the revenue cycle. However, organizations must be aware of the areas where they lack even if their margins are good because there is always room for improvement. The leaders must observe the strategies and actions of peer organizations in order to understand the factors which are playing a key role in the improvement of their revenue cycle. In addition, leaders can also take advice and help from revenue cycle consultants. This will allow them to know what is going wrong and how things can be improved. 4. Setting targets and measuring performance against those targets: Data collection, data analysis and tracking of performance measures makes more sense when financial leaders and clinicians know the targets they must achieve in terms of the KPIs. The leaders must set realistic and achievable targets for each KPI at the beginning of a fiscal year as well as monitor their progress regularly. Moreover, they must hold departments or individuals accountable for the results. 5. Using patient-centric technologies and services: Leaders must deploy patient-centric technologies which can help patients understand the billing and collection process and provide services which can allow them to make payments electronically, determine their covered benefits, estimate their out-of-pocket cost and much more. This will boost patient satisfaction and have a positive impact on reimbursements. 6. Optimizing the use of existing technologies: Some organizations don’t take full advantage of the applications available in their current revenue cycle management systems which can help in improving the performance of their revenue cycle. For example, only 44 percent of the hospitals recently surveyed by HIMSS Analytics said they use a vendor-provided claim denial management solution. 7. Focusing on claim denials: According to a study, U.S. hospitals daily write off roughly 3-4 percent of net patient revenues because of claim denials. Nobody can afford to lose revenues in such a tight market. Therefore, organizations must work smartly and focus on quality vs. quantity of work to safeguard revenues and prevent claim denials. Leaders can seek help from revenue cycle management solutions or outsource parts of their revenue cycle. 8. Focusing on patient experience: Organizations must recognize that patient satisfaction is as important as clinical excellence and it plays a vital role in driving reimbursements. Adreima, a firm which provides patient advocacy services so that patients can better understand and manage their bills and insurance, found that these types of services resulted in 29% increase in payment rates due to increased patient satisfaction. 9. Creating a culture of value for the revenue cycle: The staff should be educated about how their performance can impact the entire revenue cycle as well as influence patients’ experience. They must be informed about the KPIs so that each department or team can know their level of performance and improve in the future. Moreover, the leaders must acknowledge and celebrate the achievements of employees so that others are motivated to improve their performance. 10. Hiring the right people: It is important to hire the people who are aligned with the culture of the organization, otherwise their performance and values might influence the bottom-line. Source
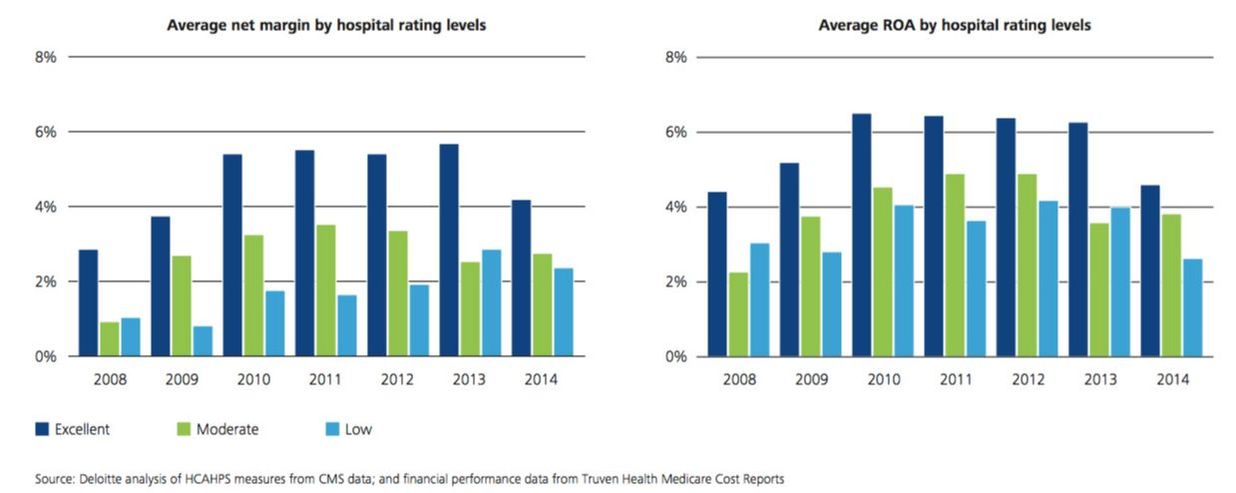
Advancement in technology and diagnostics has changed many things. Most importantly, it has shifted the focus of healthcare providers from the patients to the technology or methods which cure diseases. According to a study published in the Journal of Medical Practice Management, 96% of patient complaints are related to customer service, and only 4% are related to the quality of clinical care or misdiagnoses. Thomas Lee, chief medical officer for healthcare strategic advisory firm Press Ganey, said, “If you go back a hundred years to the time of William Osler, what it meant to be an excellent physician was to stay by the patient's bedside and really pay attention to them to help them understand what was going to happen and then relieve their suffering.” Today, patients are like customers. They have high expectations when they enter a healthcare facility and like any other consumer category, they inform their friends and family members if they are satisfied with the services provided by the healthcare facility. Their word-of-mouth helps in attracting more patients and ultimately improves the financial performance. Conversely, if patients are unhappy with the services, their word-of-mouth can significantly affect the organization’s bottom line. Moreover, patients now share their good or bad experiences with others on social media. This trend can cause greater financial damage than expected. Therefore, healthcare organizations must be abreast about the platforms where they can hear the voice of their patients and live up to their expectations. In 2007, Centers for Medicare & Medicaid Services (CMS) required hospitals to gather and submit Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) survey data in order to receive their full annual payment update. In 2013, CMS began to include the HCAHPS scores into Hospital Value-Based Purchasing (VBP) payment calculations. In fiscal year 2015 and 2016, patient experience accounted for 30 percent and 25 percent of a hospital's total performance score under VBP. Organizations with low HCAHPS scores experienced a significant impact on their bottom line. Apart from reimbursements from CMS, studies show that by improving patient experience a hospital’s financial performance is improved because it is able to attract and retain patients in such a competitive healthcare environment. A study conducted by Deloitte Center for Health Solutions found that:
Figure 1: Hospitals with excellent patient ratings have higher profitability
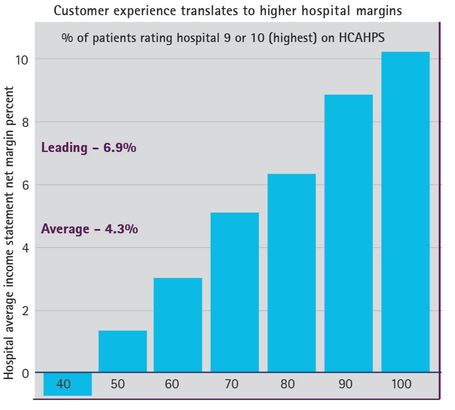
Accenture, a global management consulting, technology services and outsourcing company, analyzed hospital income margin data reported to CMS and survey results from HCAHPS and concluded that:
Figure 2: Hospitals that offer patients a better customer experience tend to have better financial performance. It is clear that healthcare organizations must shift their focus on patient experience to improve their financial performance instead of thinking of ways to reduce costs or investing capital in other projects which could increase profits.
REFERENCES
INTRODUCTION
There is no question that America’s healthcare system is dynamic and complex. With time, this industry is undergoing rapid changes because of technological innovations, new policies, more focus on patient satisfaction and other system-wide transformations. For example, the biggest change which created chaos and frustration was the replacement of paper records with electronic medical records. Healthcare organizations in U.S. as well as in other developed countries faced many challenges in order to successfully implement this change. Leaders and senior management played a major role in the incorporation of this system-wide transformation. Many healthcare leaders adopted John Kotter’s 8-steps for Leading Change to guide them throughout the change process (replacement of paper records with electronic medical records). John Kotter is recognized globally as the leading speaker and author of the topics Leadership and Change. He is an emeritus professor of organizational science and change management at Harvard Business School and conducts inspirational seminars in Executive Education programs. He is the chairman of Kotter International, a management consulting firm that guides leaders worldwide in managing change based on his 8-steps change process. His 1995 book, Leading Change, is considered as the seminal work in the field of change management. Time magazine listed this book in 2011 as one of the 25 most influential business management books ever written. Dr. Kotter has outlined 8-steps for managing change in this book which is adopted by several businesses as well as healthcare organizations for managing change. Kotter’s Change Management Theory Managers and leaders feel intimidated and uneasy while thinking about a small change to one or two processes or a system wide change to an organization. This issue can be solved if leaders adopt a holistic approach required to see the change through. After thirty years of research, Dr. Kotter proved that 70% of all major change efforts in organizations fail because leaders and managers don’t focus on how to deliver the change, where and when to start, whom to involve and how to see it through the end. There are several change management theories, but Dr. Kotter’s 8-step process has been used world-wide by healthcare organizations to implement changes successfully. The 8-steps are listed below. 1. Creating a sense of urgency Creating a sense of urgency includes efforts for developing urgency among employees, so they can feel and understand that why a change is necessary. It’s easy to manage and implement a change when the whole organization wants it. According to Dr. Kotter: "At least three quarters of management must believe that change is absolutely necessary for the transformation to work." Moreover, he wrote: "you must work really hard on Step 1, and spend significant time and energy building urgency, before moving on to the next steps. Don't panic and jump in too fast because you don't want to risk further short-term losses – if you act without proper preparation, you could be in for a very bumpy ride." 50% of the companies fail to make changes because they ignore the first step and rush to make a plan and implement it. This happens because leaders underestimate the importance of driving employees out of their comfort zones or they think that they have already done it, or sometimes they don’t have the patience to create appropriate urgency. If true urgency is created, then employees will be focused on making real progress every day that can help in achieving the goal. In addition, change initiatives fail when leaders try to win the minds or change the thinking of people by just focusing and showing the theoretical value of the change and presenting facts and figures, instead of aiming to win their hearts by changing their feelings about the situation. 2. Form a Powerful Coalition As soon as people in the organization are convinced and start talking as well as thinking about the change project, a team of influential people and effective change leaders is needed who is capable of leading and managing the organizational transformation. Dr. Kotter asserts that people who are not in favor of the change or who just pretend to support the change project must not be included in the team, because this will hurt the change process. Moreover, he suggests that people who are not in the senior management or a senior position in the organization, but always support change and do not follow the traditional company hierarchy must be included in the team. Dr. Kotter asserts that the change team must have the following characteristics:
3. Create a Vision for Change Formulating a compelling statement or in other words a powerful vision that could clearly define the desirable future and make the strategy as well as detailed decisions understandable, is important. A clear and powerful vision will help employees understand what you want from them. When employees can understand what the organization is trying to achieve, then the directions given to them will make more sense and they will be motivated to achieve organizational goals. According to Dr. Kotter: "A useful rule of thumb: If you can't communicate the vision to someone in five minutes or less and get a reaction that signifies both understanding and interest, you are not yet done with this phase of the transformation process." Powerful vision statements will have the following characteristics:
4. Communicate the vision It is important to communicate the vision in a way that catches the attention of the whole organization and maintains the sense of urgency developed in step 1 as well as motivates people to follow the directions. Under-communication of the vision often results in the failure of the change project. Studies show that most companies under-communicate their vision by at least a factor of 10. Memos, e-mails, special meetings, and speeches given by the CEO or the change team at occasions are not enough. Communication of the vision will have a competition with other things communicated on a daily basis. Therefore, in order to keep the vision fresh in the minds of the employees, everything – presentations, meetings, problem-solving, decision making, speeches, company newsletters, training, e-mails, daily activities etc. – must be tied to the vision. In other words, the senior management and change coalition must use every effective communication channel to broadcast the vision of the organization. Moreover, the communication style should be creative enough to win the hearts of the employees or connect to their deepest values, so that the employees are motivated to accept the change. Another important thing is to “walk the talk”. Leaders and managers must lead by example and communicate the vision through their actions. A communication program is undermined if the leaders and the change coalition do not back up their words with behavior. When an entire team of senior management demonstrate the change they want to see, it increases motivation, inspires confidence and decreases skepticism. 5. Remove Obstacles At this stage, an organization must have incorporated the change vision in all aspects and hopefully convinced people from different levels to participate in the change project. As more and more people struggle to achieve the goals, they might encounter certain obstacles that halt their progress or hinder the change management process. Therefore, it’s important to remove barriers that dis-empower people and makes the change process slow. The barriers might be the supervisors, the system, mental walls, and lack of information. Troublesome supervisors are notorious for hindering the change process. Their management style is quite different from what is required to easily adopt the change. It’s difficult to change their behavior. The best solution is honest dialogue. Moreover, A system which fails to reward and promote people who successfully adopt the proposed changes must be modified, otherwise it may discourage people from progressing. Physicians, nurses, radiologists, etc. might think that the proposed changes are not practical or they are so complex that no matter how much effort they put in, the organization won’t be able to survive the changes. These are mental walls which don’t allow people to adopt the change. The change coalition can call consultants or people from other organizations who successfully survived the changes in order to convey the message that ‘‘I survived this type of change, you can too.’’ The last barrier could be lack of appropriate information. Proper information can help people in decision making and improving their performance. Accurate and timely feedback about the level of performance will motivate people to improve. Otherwise, some might think that they are performing at a high level. If that is not the case, then the change process gets slow. 6. Create Short-Term Wins Setting of short term goals is necessary because it breaks the change project into simple and achievable steps as well as provides a framework which can be easily understood and followed by employees to achieve the final goal. Short term goals should be clearly related to the core changes being sought after. The short term wins must be rewarding for the employees, so that they are motivated to achieve them. Moreover, the short-wins will help boost employee morale, enabling them to put extra effort in the future. According to Dr. Kotter: "Most people won't go on the long march unless they see compelling evidence in 12 to 24 months that the journey is producing expected results." In addition, achievement of short-term goals frustrate the opponents of the change project, thus making it difficult for them to criticize and hinder the process. On the other hand, proponents get more support from the senior management. This may lead to the buying-in of more people who were hesitant before in joining the change process. Nevertheless, the short term goals are hard to come by. They need careful planning and efforts to materialize. Lack of commitment, lack of enthusiasm plus poor management by key people may lead to the creation of irrational short-term goals which are hard to achieve and imagine. If this is the case, then people will fail in achieving the short-term wins and this might lower their morale as well as allow the opponents of the change process to demotivate them and criticize the change initiative. 7. Build on the Change Quick wins are just the start of what should be done to accomplish long-term change. Real change runs deep. Following success in the previous stages, failure or challenge is eminent when you don’t expect it. However, leaders should not give up. They must chase their dream. They must not allow failure to sink them back because starting all over again is hectic. Leaders must encourage continuous progress reporting, highlight achieved and future milestones, examine what went right and what needs improvement, set goals to continue building the momentum achieved in the past and, keep ideas fresh by including new change agents and leaders in the change team in order to instill the changes into the organization and make sure the practices are firmly rooted in the organization’s culture. This will help them in building the change. 8. Anchor the changes in corporate culture The new practices which helped in the successful implementation of the change, must be deeply rooted in the organization’s culture. Success must be clearly seen and well communicated. However, on the way some people will leave the organization. Hence, reinforcing the new recruits on the culture of the organization is essential. It is important that the company’s leaders and senior management continue to support the change. This includes old and new staff members. The change team and leaders must:
References
The demand for value-based care which controls costs and focuses on quality has resulted in a shift from fee-for-service payment system to bundled payments in healthcare. Fee-for-service payment system has been popular for a long time. The providers bill the patients for every service they provide and therefore this system promotes quantity over quality. On the other hand, bundled payments help in aligning financial and quality of care incentives, but how?
Basics of Bundled Payments According to the bundled payment model, a single payment is given to the multiple providers or healthcare organizations who provide services to a patient for a single episode of care. Episode of care is the time period for which a patient with a certain disease undergoes several treatments and receives services from multiple providers. For example, if a person undergoes a hip replacement surgery, the payer will collectively reimburse the providers using a price determined from previous financial records, instead of reimbursing the surgeon, anesthesiologist, etc., separately. In 2013, the Centers for Medicare & Medicaid Services (CMS) established the Bundled Payment for Care Improvement (BPCI) program for controlling healthcare expenditures and assuring quality care to the beneficiaries. The program comprises of four models (consist of 48 different types of episodes of care) on the basis of which the providers receive a lump sum amount of money for the services rendered to patients. The participants of BPCI must meet the quality standards and stick to the set price for each episode of care. If the cost of care is higher than the set bundled price, the organization will bear the financial burden. On the other hand, if the cost of an episode of care is lower than the set bundled payment, then the organization can keep the difference. This motivates the providers to coordinate and make cost-effective as well as high quality care decisions for the patients. In other words, the providers are accountable for their performance as well as the expenditures of episodes of care under the bundled payment system. Under the bundled payment model, either the payer reimburses a single organization which then distributes payments among the providers or it pays each provider separately in a way that the set price in not exceeded. Success of the Bundled Payment Model In 2013, Medicare saved $42.3 million on bypass patients treated in the demonstration hospitals. The Cleveland Clinic Euclid Hospital saved $1.65 million for total hip arthroplasty (THA) and total knee arthroplasty (TKA) by joining BPCI. The readmissions for THA decreased from 5.8 percent to 4.8 percent in 2014, and to 4.0 percent by 2015. For TKA, the overall readmissions dropped by 30 percent in 2015. In the private sector, Blue Cross and Blue Shield of North Carolina (BCBSNC) introduced a bundled payment system for knee replacement in 2011. One episode of care consisted of pre-surgical period of 30 days prior to hospitalization, the surgery, and follow-up care of 180 days after discharge from the hospital. In a period of one year, BCBSNC saved on average 8 to 10 percent per episode. Geisinger Health System has established a performance-based bundled payment model called ProvenCare, which reimburses providers for coronary artery bypass graft surgery (CABG). The model achieved the following results: a 10 percent reduction in readmissions, reduced average length of stay, and reduced hospital charges. Since then, Geisinger has added the following episodes to ProvenCare: elective coronary angioplasty (PCI); bariatric surgery for obesity; perinatal care; and treatment for chronic conditions. How to Succeed in the Bundled Payment Model? The major element for the bundled payment system to be successful is the strong communication between the providers. Based on the goals to be achieved, the providers must communicate and design efficient care coordination strategies. They must ensure that cost-effective decisions are being made at every level of the episode and high quality care is being provided to the patient. Providers can predict the needs of those patients who are less sick, whose care is inexpensive and whose treatment is easy to predict. By doing this, they can make sure that the cost of their episode falls into the set price of the bundled payment. Moreover, providers must understand the risks associated with those patients who are extremely sick because more resources would be needed to restore their health. Challenges Associated with Bundled Payment System A significant challenge with bundled payments is that it may be impossible for a provider to manage the costs associated with an episode of care. For example, the patients might be involved in risky behaviors, they might have several comorbidities which could complicate the situation, they might be at a high risk due to which their treatment would be expensive, etc. All these things are not in the control of the providers and may result in expenditures which are above the set bundled payment. The successful implementation of the model also requires a robust health IT system with comprehensive reporting or data collection tools. Without a strong IT system, the entities won’t be able to analyze their performance, quality improvements and cost effectiveness, efficiently. References
|